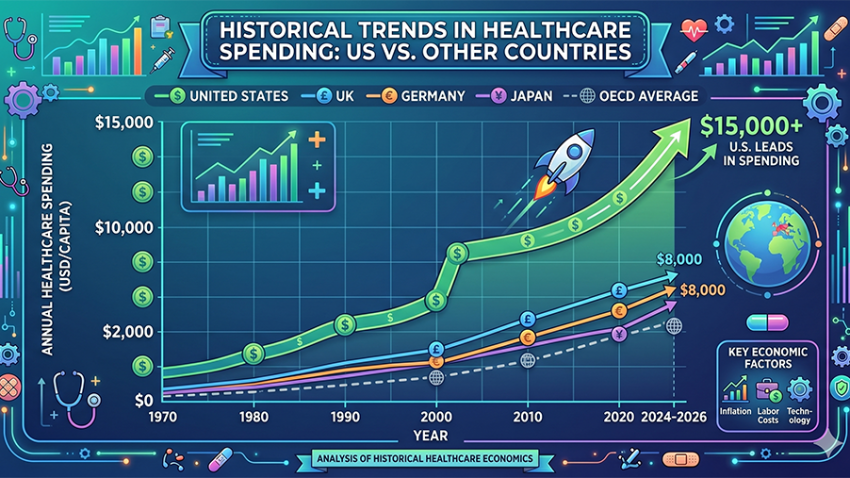
The Price of Wellness: Why U.S. Healthcare Costs Are in a League of Their Own
In the global landscape of medicine, the United States stands out—not just for its cutting-edge research and world-class specialists, but for a price tag of healthcare costs that dwarfts that of every other developed nation. As we move through 2026, the gap between American healthcare spending and that of its international peers continues to be a central point of economic and political debate.
To understand the current crisis, we must look at how the U.S. compares to the rest of the world and how we reached this record-breaking financial peak.
The Global Comparison: A $15,000 Per Person Reality
Data from 2024 and 2025 reveals a staggering disparity. While all wealthy nations have seen costs rise following the COVID-19 pandemic, the U.S. remains the undisputed leader in spending.
| Country | Healthcare Spend Per Capita (2024) | % of GDP (2024) |
| United States | $14,775 | 17.2% |
| Switzerland | $9,963 | 11.5% |
| Germany | $9,365 | 12.0% |
| Netherlands | $8,436 | 10.1% |
| OECD Average | $7,860 | 9.2% |
On average, the U.S. spends nearly double what other high-income countries (like the UK, Canada, and Australia) spend per person. Despite this, the U.S. often lags behind these peers in key health metrics, including life expectancy and the prevalence of chronic diseases.
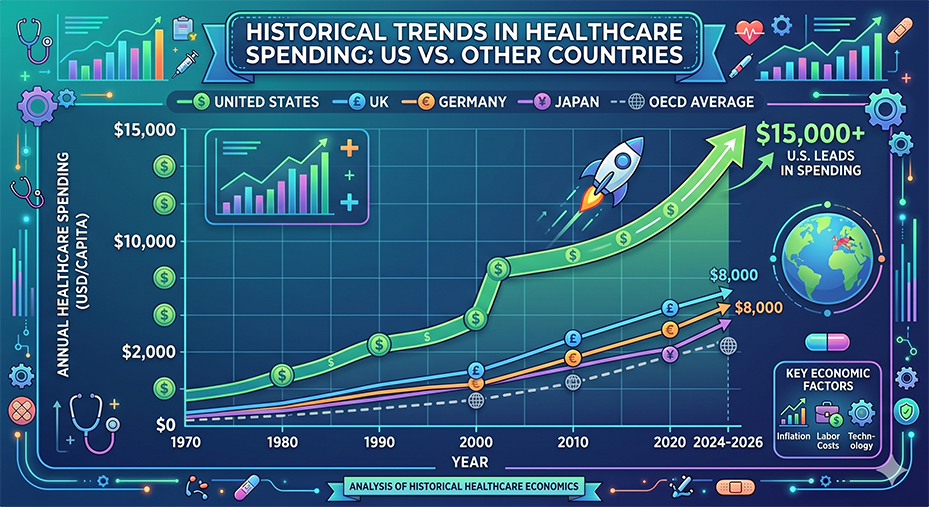
The Historical Climb: 1970 to Present
The astronomical cost of modern American healthcare didn’t happen overnight. It is the result of a steady, decades-long climb that has consistently outpaced the growth of the overall economy.
- 1970: The U.S. spent just $74.6 billion on health, roughly $353 per person. Healthcare accounted for only 6.9% of the GDP.
- 2000: Costs crossed the trillion-dollar mark ($1.4 trillion), representing about 13.3% of the GDP.
- 2024: Total national health expenditures reached nearly $5.3 trillion, or $15,474 per person (when including all research and infrastructure).
Historically, health spending growth has outpaced GDP growth by several percentage points almost every decade. While the 2010s saw a slight “cooling off” period with average annual growth of 4.2%, the post-pandemic era (2020–2026) has seen a resurgence in spending, driven by labor shortages, pharmaceutical breakthroughs, and a backlog of deferred care.
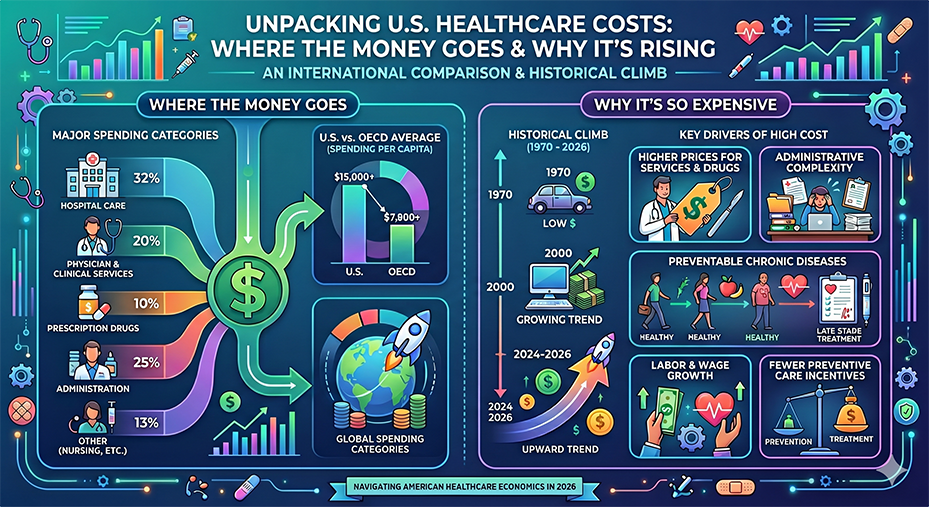
Why is it so Expensive?
If the U.S. isn’t necessarily seeing doctors more often (in fact, Americans have fewer physician visits per year than the OECD average), where is the money going? Experts point to several “uniquely American” drivers:
1. Higher Prices for Services and Drugs
In most countries, the government negotiates price caps for medical procedures and medications. In the U.S., a fragmented system of private insurers leads to wildly varying and much higher prices. For example, the U.S. spends over $8,000 per person on inpatient and outpatient care alone—more than many countries spend on their entire health system.
2. Administrative Complexity
The U.S. system requires a massive “middleman” workforce to manage billing, insurance claims, and multi-payer negotiations. Administrative costs account for about 15–25% of U.S. healthcare spending, compared to low single digits in countries with simplified or single-payer systems.
3. The “Treat Over Prevent” Model
The U.S. allocates a smaller fraction of its budget to public health and prevention compared to its peers. Approximately 90% of spending is driven by chronic diseases (like diabetes and heart disease) that are often treated at advanced, expensive stages rather than managed through early, low-cost intervention.
4. The Baumol Effect and Labor Costs
Healthcare is a labor-intensive industry. As wages rise in the general economy, healthcare wages must follow to attract talent—but unlike manufacturing, a surgeon cannot “automate” a surgery to increase productivity in the same way. This leads to a natural, steady rise in costs known as the Baumol Effect.
The Shift in Who Pays
In 1970, patients paid about 33% of their medical costs out-of-pocket. Today, that share has dropped to roughly 10%, with the difference being made up by public insurance (Medicare/Medicaid) and private employer-sponsored plans.
While this sounds like a win for consumers, the “hidden” costs are enormous. Higher healthcare spending manifests as lower wage growth for workers (as employers spend more on premiums) and higher taxes to fund government programs.
Conclusion
As the U.S. healthcare bill continues its upward trajectory toward 18% of GDP, the conversation is shifting from access to affordability. Without structural changes to address the underlying prices of service and the administrative weight of the system, the U.S. will likely remain an outlier—paying the world’s highest prices for a system that many argue still leaves too many behind.
Keep Reading
If this was useful, you’ll probably like these too:









Leave a Reply